Content
- What is hemorrhagic vasculitis
- Hemorrhagic vasculitis – ICD code 10
- Causes of hemorrhagic vasculitis
- Hemorrhagic vasculitis – symptoms
- Hemorrhagic vasculitis – forms
- Vasculitis – stages
- The course of hemorrhagic vasculitis
- Diagnosis of hemorrhagic vasculitis
- Treatment of hemorrhagic vasculitis
- Diet for vasculitis
- Complications of Vasculitis
In childhood or adulthood, acute inflammation of the vessels with an extensive lesion of the digestive tract, skin, kidneys, joints can suddenly begin. A hemorrhagic rash appears on the body, and the disease is officially called vasculitis. It is important to start conservative treatment in time, otherwise serious health complications will progress.
What is hemorrhagic vasculitis
The second name of the specified diagnosis is Shenlein-Genoch disease, which begins with an acute stage. Relapse often occurs at the age of 4-12 years, is a serious complication of scarlet fever, sore throat, SARS. During the pathological process, the walls of the capillaries under the influence of provoking factors become brittle, their permeability increases. The microvasculature and the chemical composition of this biological fluid are disrupted: platelet activation, decrease in antithrombin concentration, blocking of fibrinolysis activators.
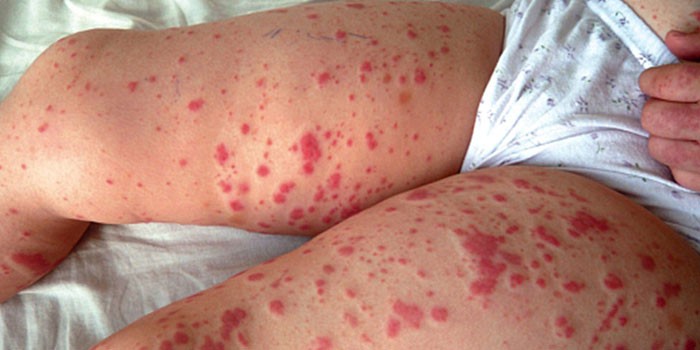
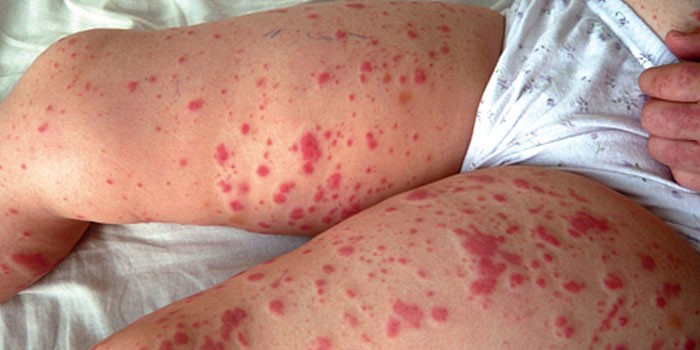
A vascular network appears on the skin, extensive hematomas with fuzzy borders form. Externally, hemorrhagic vasculitis resembles an allergic reaction. Rheumatic purpura in practice is not common, prone to chronic transformation. It occurs due to an increased tendency to an allergic reaction, against the background of insufficient blood coagulation, other provoking factors are not excluded. Moreover, in the body there is a violation of hemostasis of the vascular link, a tendency to hypercoagulation.
Hemorrhagic vasculitis – ICD code 10
Hemorrhagic vasculitis in the international classification of diseases (ICD) is declared by doctors as allergic purpura. Before making a final diagnosis, a complete clinical examination is shown, a series of tests are performed. According to the symptoms, the disease is represented by allergies, according to the etiology it has an inflammatory, progressive character. The danger lies in the fact that not only the skin vessels, but also the vessels of the parenchymal organs are involved in the pathological process. Purple Schoenlein-Genoch, on average, affects 25 patients aged 5-14 years per 10,000 people.
Causes of hemorrhagic vasculitis
Without finding out the etiology of hemorrhagic vasculitis, it is impossible to achieve complete
patient recovery. Otherwise, the number of seizures only becomes more frequent, and skin rashes become large-scale, intoxication of internal organs and systems is observed. Therefore, in order to cure the disease, it is required to find out the main causes of vascular inflammation. It:
- increased activity of infectious agents;
- preventive vaccination (antibody formation);
- hypothermia of the body;
- burn disease;
- congenital insufficiency of the complement system;
- autoimmune diseases;
- capillarotoxicosis during pregnancy;
- genetic predisposition;
- food poisoning;
- upper respiratory tract infection;
- prolonged exposure to the sun;
- tendency to allergic reactions;
- harmful insect bites.
Vasculitis in children
Since the disease develops more often in childhood, parents should exclude the child from the risk group, reduce the risk of the first attack, pay attention to the initial symptoms of hemorrhagic vasculitis. The pathological process starts, like an allergic reaction with a small skin rash. If it is not stopped, pediatricians do not exclude angioedema, other complications.
Hemorrhagic vasculitis in children begins with symptoms of general malaise, which are complemented by acute abdominal pain, a complete lack of appetite, fever, and inflammation of the knee and elbow joints. After some time, rashes, signs of hyperemia of the skin appear on the skin. Symptoms of a hemorrhagic form of the disease are similar to dermatitis.
Hemorrhagic vasculitis in adults
In older patients, the disease prevails extremely rarely, but in case of relapse requires a therapeutic diet. Additional hospitalization on the recommendation of the attending physician is not necessary. Symptoms are milder, and abdominal syndrome is observed in 50% of the victims, while not accompanied by vomiting, nausea. Hemorrhagic purpura in adults with kidney damage is fraught with the development of renal failure, diffuse glomerulonephritis.
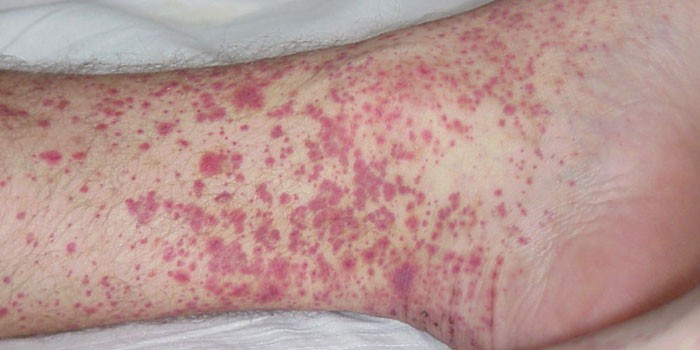
Hemorrhagic vasculitis – symptoms
Hemorrhagic purpura begins with a general malaise, which reduces the patient’s quality of life. Before vasculitis appears on the skin, body temperature may increase, signs of acute respiratory viral infections are not ruled out. Later, the diagnosis can be differentiated, since extensive foci of skin rash become a specific symptom. To correctly determine the diagnosis of ICD, the doctor collects anamnesis data, listens to complaints in a specific clinical picture. More often with hemorrhagic purpura this is:
- joint syndrome;
- spotty small rash;
- skin syndrome;
- myalgia;
- abdominal syndrome;
- extensive kidney damage.
In addition, the patient should pay special attention to such changes in the general well-being of a sick child, for example:
- soreness of movements;
- feces with impurities of blood;
- nausea and vomiting;
- dizziness;
- fainting state;
- tachycardia attacks;
- blood impurities in the urine;
- acute glomerulonephritis.
Hemorrhagic vasculitis – forms
Since the disease demonstrates a systemic effect in the body, doctors distinguish its classification in accordance with the established ICD standards. All existing forms of hemorrhagic vasculitis have specific symptoms, so they significantly facilitate the diagnosis of the disease. Self-medication and diagnosis at home are strictly prohibited. The etiology of the pathological process distinguishes these types of hemorrhagic vasculitis:
- cutaneous;
- cutaneous and articular;
- abdominal;
- renal;
- mixed.
By the duration of the inflammatory process, the intensity of symptoms, these forms of hemorrhagic vasculitis are distinguished:
- spicy;
- protracted;
- chronic.
Vasculitis – stages
The skin hemorrhagic syndrome in the photo terrifies patients, therefore it is better not to bring to complications, to exclude the need for resuscitation measures. To do this, it is useful to find out what stages of the disease exist, how they appear in practice, how they characterize the prevailing clinical picture. So, allocate:
- initial stage (mild);
- moderate stage;
- severe hemorrhagic vasculitis.
The course of hemorrhagic vasculitis
Studying the duration of the pathological process, doctors distinguish another conditional classification, which also characterizes the pathogenesis of rheumatic purpura. So, the course of hemorrhagic vasculitis covers the following time intervals, which gradually replace each other in the absence of positive dynamics:
- acute course in which vasculitis progresses throughout the month;
- subacute with a duration of pathology up to 3 months;
- protracted when vasculitis is not treated until six months;
- recurrent with systematic repetitions of the acute stage;
- chronic course with a medical history of more than 1.5 years;
- fulminant course of the disease lasts less than 5 days, appears only in a small child.
Diagnosis of hemorrhagic vasculitis
To determine a characteristic ailment in the body, a complete examination is necessary. Diagnostics includes not only instrumental methods, but also laboratory tests with the subsequent implementation of all the recommendations of a specialist. So, in order to make a final diagnosis of hemorrhagic vasculitis, it is necessary to perform:
- General blood analysis. Leukocyte jump, ESR, decrease in hemoglobin, red blood cells, production of neutrophils by the cells of the phagocytic system.
- General urine analysis. Especially relevant in renal syndrome, when secondary activation of proteins is observed.
- Blood chemistry. A sharp jump in the concentration of sialic acids, haptoglobulin, fibrinogen. Additionally, you can determine the level of creatinine, cholesterol, uric acid.
- Immunological examination for the occurrence of a pathological process in the body, for differential diagnosis.
- Ultrasound, endoscopic methods and a biopsy of the affected organ – as necessary to detect the same multiple microtomy formation.
Treatment of hemorrhagic vasculitis
If symptoms of aseptic inflammation are evident, it is important not to hesitate with the start of intensive care. An integrated approach is required, which includes taking medication, bed rest and a therapeutic diet containing only hypoallergenic foods. Folk remedies for hemorrhagic vasculitis have a mediocre effect, can only complement official methods.
Before treating hemorrhagic vasculitis, it is important to understand that it is necrotic thrombovasculitis, rheumatic vasculitis, hemovasculitis, microtrombovasculitis, panvasculitis or rheumatic purpura. Only after the final diagnosis is made, the doctor prescribes medications, additionally recommends physiotherapy. If spontaneous remission predominates, this does not mean at all that it is necessary to stop intensive therapy earlier than the established deadline..
Medication for vasculitis
It’s worth starting with taking medication. Hemorrhagic vasculitis is treated successfully if the drugs are correctly selected, i.e. they should be fully consistent with the prevailing clinical picture. The following is an intensive care regimen:
- Receiving enterosorbents to eliminate intoxication products. These are drugs Enterosorb, Enterosgel, Polyphepan, activated carbon.
- Disaggregants. Necessary to improve blood microcirculation. With hemorrhagic purpura, this is Curantil, Ticlopidine, Trental.
- Anticoagulants to reduce puffiness, prevent the formation of blood clots. This is Hepatrombin, Heparin.
- Glucocorticosteroids are effective in renal and articular syndromes of hemorrhagic purpura, relieve the inflammatory process. This is methylprednisolone, prednisolone.
- Antibiotic agents for suppressing infectious pathogenic flora in hemorrhagic purpura.
- Cytostatics for strengthening immunity and prevention of malignant tumors, as an option Cyclophosphamide, Endoxan.
- Immunosuppressive drugs to enhance the body’s immune response to pathogenic flora in hemorrhagic purpura. This is Azathioprine, Imuran.
- Antihistamines to suppress the external signs of rheumatic purpura, which can occur in acute form. This is Tavegil, Suprastin, Supradin.
- Membrane stabilizers to accelerate the process of regeneration of damaged tissues. These are vitamins such as nicotinic acid, rutin, tocopherol.
- Infusion infusion of solutions obtained from body fluids, such as plasma.
- Plasmapheresis.
Vasculitis treatment folk remedies
Aseptic inflammation can be eliminated by the methods of alternative medicine, however, such treatment is mediocre. It can complement official methods, take part in the rehabilitation period. So that the treatment of vasculitis with folk remedies is as effective as possible, it is recommended to prepare the following ointment with the active components of plant origin:
Grind birch buds in an amount of 200 grams, add so much fat of nutria so that a homogeneous composition of a viscous consistency is obtained. Insist in the refrigerator, and with daily use, rub the affected lower limbs, hands, other manifestations of palpable purpura on the body. This is an effective treatment for systemic vasculitis, which can be supplemented by taking medications as recommended by a specialist..
Diet for vasculitis
Anaphylactoid purpura is treated with proper nutrition, therefore, allergic foods must be completely excluded from the daily diet. The diet for hemorrhagic vasculitis includes the use of therapeutic decoctions, but the use of the following products in the daily menu is strictly contraindicated:
- salt in large quantities;
- coffee, alcoholic beverages;
- hot or cold water, food;
- any seasonings and spices;
- potassium-containing foods;
- refractory fats.
Complications of Vasculitis
An untreated disease in a timely manner exacerbates the clinical picture. Complications of hemorrhagic vasculitis already require immediate hospitalization with resuscitation in order to eliminate a large concentration of allergens and toxins from the body. This is what causes aseptic inflammation in a patient at any age:
- posthemorrhagic anemia;
- Iron-deficiency anemia;
- perforation of stomach and intestinal ulcers;
- intestinal obstruction;
- peritonitis;
- DIC syndrome with thrombocytopenia;
- pancreatitis
- thrombosis, thrombopenia;
- atherosclerosis;
- cerebral paralysis.